Antimicrobial resistance: the problem
Written by Poppy Pescod, March 31st 2020
Bacteria that cause infectious diseases are often treated with antibiotics – a group of medicines that specifically target bacteria, reducing or clearing an infection. The first antibiotic, penicillin, was discovered by Alexander Fleming in 1928; mass production and administration of penicillin saved thousands of lives during World War II, leading it to be called ‘the wonder drug’. Antibiotics have been used regularly to treat medical and veterinary bacterial infections since the 1940s.
Unfortunately, some bacteria are naturally resistant to antibiotics. When a bacterial infection that contains a few resistant bacteria is treated with antibiotics the resistant bacteria will flourish, causing an infection that can’t be treated with antibiotics. Resistance to antibiotics comes in many forms, using many different mechanisms, and can spread between bacteria on floating pieces of DNA (known as horizontal gene transfer). Image credit: NIH NIAID.
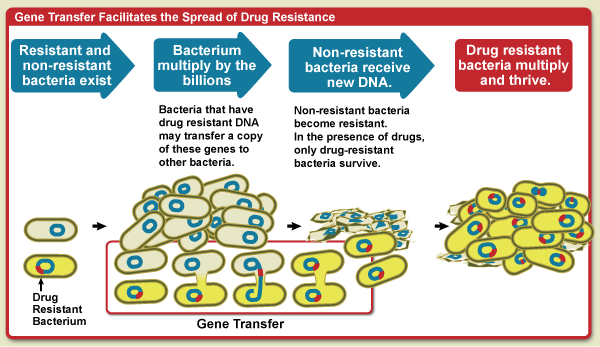
People taking antibiotics unneccessarily, or not finishing antibiotic treatment courses, has resulted in antimicrobial resistance (AMR) becoming widespread in humans and animals. In many countries antibiotics can be bought over-the-counter without a prescription. This has lead to people taking only what they can afford rather than a full course, and taking antibiotics when they don’t need them. We have now reached a stage where resistant forms of bacteria, such as MRSA, are killing an estimated 700,000 people a year, with that number expected to rise to 10 million by 2050 if no action is taken.
Antimicrobial resistance: the solution
With the right intervention strategies and research support, AMR can be controlled. Increasing awareness of public health, improving access to clean water in developing countries and better government controls over the sale of antibiotics will reduce the spread of AMR. Research into discovering new antibiotic classes, antibacterial alternatives, and monitoring of AMR will be critical to its reduction.
As a global challenge, AMR requires a global response. In 2015 the World Health Organization published a global action plan to unite researchers, clinicians and the pharmaceutical industry in the fight against AMR.
Antimicrobial resistance is a crisis that must be managed with the utmost urgency. As the world enters the ambitious new era of sustainable development, we cannot allow hard-won gains for health to be eroded by the failure of our mainstay medicines.
Dr Margaret Chan, Director-General of the World Health Organization, 2015